A global scan of mental health policy responses for long-term care home residents during COVID-19

Compiled by the Oxford COVID-19 Government Response Tracker and the International Network for Government Science Advice (INGSA)
Introduction
Elderly people have been of particular interest to policymakers during the COVID-19 pandemic. They have comprised a significant proportion of COVID-related cases and deaths in multiple countries, and residents have been particularly vulnerable due to their age and pre-existing comorbidities.
This has led to extensive protections being introduced into long-term care facilities (LTCFs) for the elderly, to reduce transmission and protect elderly people from COVID-19. These protective policy responses have fallen into three main categories:
- limiting or prohibiting visitors;
- isolating symptomatic residents; and
- increased hygiene and infection controls.
The Oxford COVID-19 Government Response Tracker (OxCGRT) currently suggests that at least 45% of countries, regions and territories have introduced extensive protections for elderly populations – both in the community and within residential care settings – during the last 14 months (see Figure 1). Existing vulnerabilities to COVID-19 mean the impacts of increased fear, social isolation, and disruption to normal routines have been exacerbated, and public health interventions have consequently been called for to aid elderly people in LTCFs.
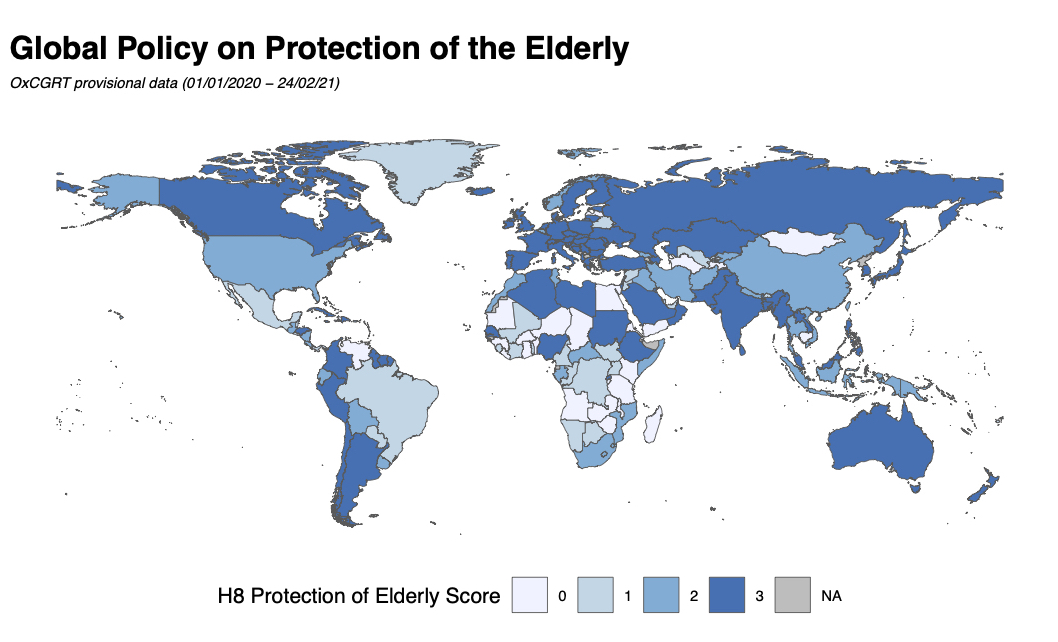
Figure 1: Choropleth map showing the strength of policies designed to protect elderly people by isolating them from potential exposure to COVID-19, based on the OxCGRT indicator H8. (0 = no policy, 1 = recommendations of protection; 2 = narrow protection; 3 = wide protection)
National governments have introduced different policies to mitigate the harmful impacts of extensive care home restrictions on the mental health and wellbeing of elderly residents. This note includes information collected by contributors to both the OxCGRT and International Network for Government Scientific Advice (INGSA) research groups.
A total of 85 countries were surveyed across all regions of the world. From these countries, 13 policies were identified relating to mental health interventions in LTCFs. Several countries introduced specialist mental health provisions for elderly residents in the community setting (not LTCFs); however, these policies were deemed to be outside of the remit of this evidence can. For 72 countries, no relevant policies in this area were identified.
Policies to improve mental health and wellbeing in LTCFs can be grouped by several key themes: the provision of telemedicine; community volunteers conducting phone calls; remote digital technology to communicate virtually; specific training for LTCF staff; and increasing paid leave for caregivers.
Telehealth
Telehealth and teleconsultations are a common strategy to mitigate the mental health impacts of COVID-19, and have increased in popularity over the past year. These consultations have led to an increased ability for elderly residents of LTCFs to receive remote care and advice without being placed at risk of infection.
- In Australia, an increase in budget was given in November 2020 for the Medicare Better Access to Psychiatrists, Psychologists and General Practitioners programme. This increased access to GP services, mental health treatment and counselling for patients in LTCFs.
- In Germany, tablets were provided to enable virtual GP visits for residents. These were used to reduce stress around potential infection risks, and allow access to medical services (including psychotherapy) throughout lockdown.
- Iceland invested several billion Króna in measures to counteract social isolation and increase telemedicine services to support elderly people.
- In Slovakia, social counselling services for the elderly were provided using phone infolines run by the Public Health Authority of the Slovak Republic, the Ministry of Labour, Social Affairs and Family, and the Ministry of Interior.
- In the Philippines, the state-run National Center for Mental Health (NCMH) launched the Telemental Health Response programme, an online platform for remote psychosocial services, to help vulnerable segments of society including elderly communities cope better with pandemic-induced stress and anxiety. The programme, while not necessarily catering specifically for senior citizens, allows LTCF residents to access psychosocial services remotely.
Community check-in phone calls
- In Australia, AUD$10 million was given to the Community Visitors scheme, seeking to target social isolation by connecting elderly people, including residents of government-subsidised residential aged care, on the telephone and via the internet to their loved ones with the help of trained volunteers.
- Ireland’s government launched a ‘community call’ to activate formal and informal networks that could check in and support vulnerable people who were isolating and at risk of loneliness. Volunteer networks were set up on a national volunteering database, I-VOL, which was used to recruit community volunteers; phone hotlines were also set up. Between April and June 2020, more than 10,000 social isolation calls were made.
Technology to enable virtual communication with family
- In Germany, tablets were also used to enable ‘virtual visits’ to LTCFs, allowing residents to communicate both with family members and other residents, with the aim of reducing loneliness and isolation.
- Singapore introduced a national policy to improve (i) care home access to technology for connection on digital platforms, and (ii) senior citizen technology literacy, in order to allow them to connect with their families remotely.
- In New Zealand, an independent review recommended increasing staffing in LTCFs to develop the use of technology for both pharmaceutical management and to establish online communications (via Facebook and Whatsapp groups) – both among residents, and between residents and their families. The review found that the higher the level of government restriction policy, the higher the level of attention to psychological wellbeing of residents was required. Another initiative, The Better Digital Futures for Seniors programme, trained older New Zealanders to use digital methods to communicate. This was not just for residents of LTCFs, but also for those in the community.
Specific training for LTCF staff
- South African guidance for mental health and wellbeing in LTCFs recommended establishing a team, or dedicating a staff member, to provide emotional support for both staff and residents – in particular, to encourage conversations on fears and frustrations.
- In India, the National Institute of Mental Health and Neuroscience published guidance for mental health in LTCFs for the pandemic. Education was given to practitioners on both recognising a range of mental health disorders caused by the increased isolation (anxiety, depression, insomnia, delirium and acute psychosis), as well as how to treat them pharmaceutically.
- National government ministries in Indonesia also published guidelines on senior citizen mental health service provision during COVID-19. These included: providing companion staff for the elderly; providing motivation to instil optimism and keep elderly people in good spirits; and guidance on teaching the elderly how to use technologies to communicate digitally and remotely.
- New Vietnamese LTCF mental health guidelines were introduced which highlighted: maintaining social connectedness; ensuring adequate lighting in living residences; recommendations on stimulating activities and hobbies; and improving spiritual life.
Financial support for family members to deliver care
- Luxembourg introduced leave for family support to enable employees and self-employed people to look after elderly persons following the closure of psychogeriatric senior centres. The terms of the scheme meant that leave for family support could be requested from 25 June 2020 up to 24 May 2021. Leave for family support runs until the approved care structure notifies the minister that it has resumed all or part of its activities, and that there is a place available in the approved service for the person concerned to return to.
Further reading: The mental health and wellbeing of care home residents and staff: a snapshot of impacts and responses
Appendix
Contributors to this global evidence scan
Andrew Wood, Helen Tatlow, Victoria Cavero, Ayanna Griffith, Tiwalade Ighomuaye, Israa Mohammed, Kaitlyn Myers, Tim Nusser, Syed Shoaib Hasan Rizvi, Kaisa Saarinen, Ellen Sugrue, Naomi Simon-Kumar, Kristoffer Berse, Tomáš Michalek, Muhammad Djindan, Pradeep Kumar, Trang Nghiem Nguyen Minh, Lianne Angelico Depante
Summary of policy responses
| Country | Response |
| Australia | AUS$10 million for virtual visits using phone and internet. |
| Germany | Providing LTCFs with (free) tablets and training to facilitate virtual meetings for residents. |
| Iceland | Measures to counteract social isolation among the elderly and in telemedicine. |
| India | Published guidance for practitioners to support mental health during the pandemic. |
| Indonesia | Guidelines for care home staff, companion staff, and in the use of digital communications technology. |
| Ireland | Telemedicine and community volunteers making isolation telephone calls. |
| Luxembourg | Paid leave for family members to support elderly relatives following care home closures. |
| New Zealand | Increased provision of remote digital communication technology. |
| Philippines | Provision of remote psychosocial services on an online platform. |
| Singapore | Improving access to remote digital technology for communication. |
| Slovakia | Social counselling provided on phone lines. |
| South Africa | Trained LTCF staff in delivering emotional wellbeing support. |
| Vietnam | Guidance on lighting, social connectedness, and spiritual life. |
